Dental occlusion
Tooth occlusion
Dental occlusion refers to the way the teeth of the upper and lower jaws come into contact when we close our mouth, swallow, and chew. Simply put, it describes how our teeth “fit together.”
Occlusion does not involve only the teeth. It also affects the jaw, the temporomandibular joints (TMJ), the muscles of mastication, and ultimately the overall comfort and function of the mouth in daily life.
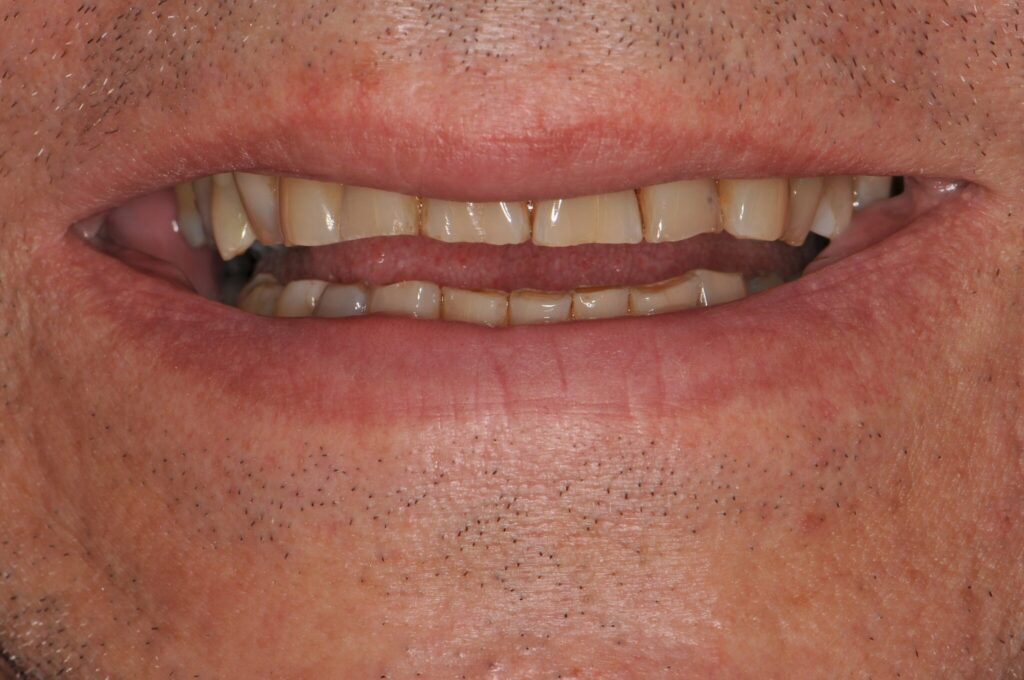
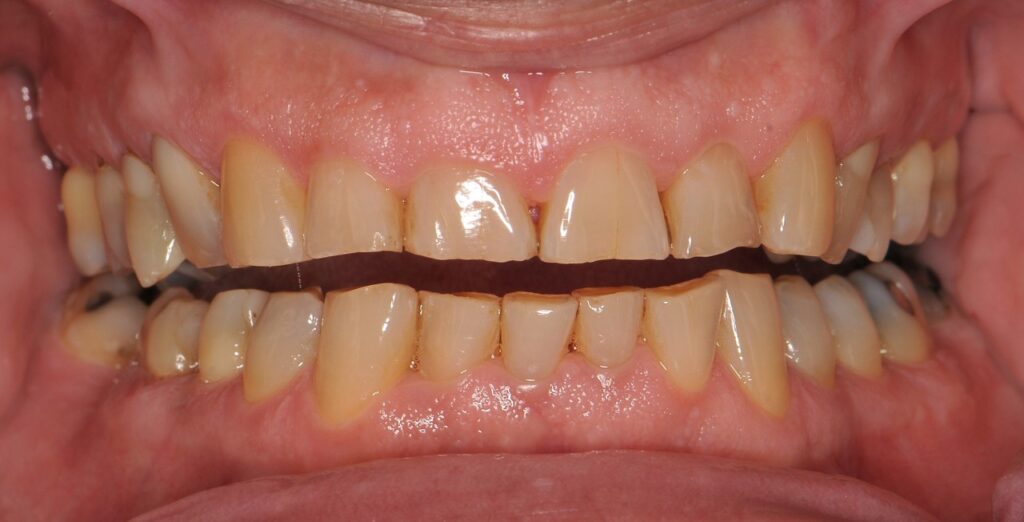
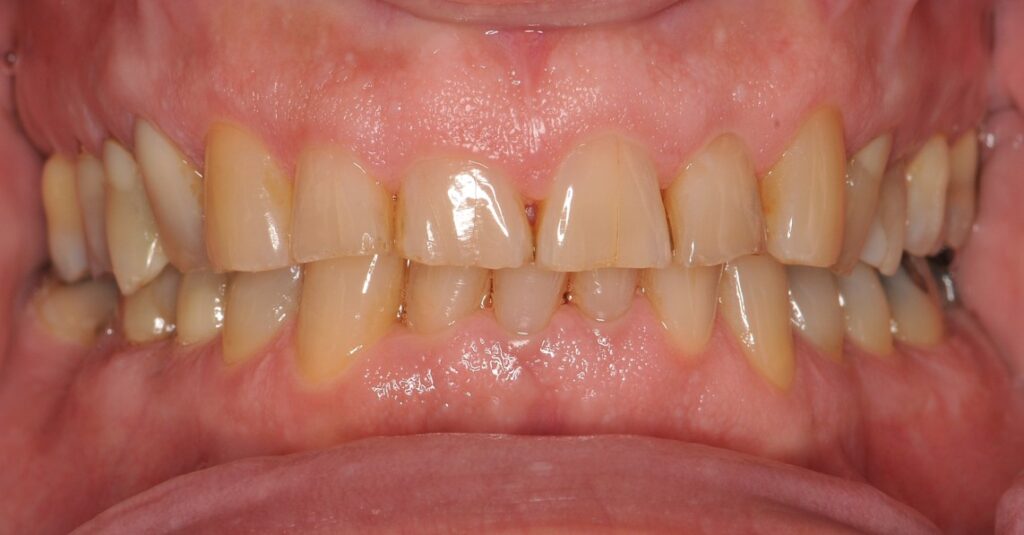
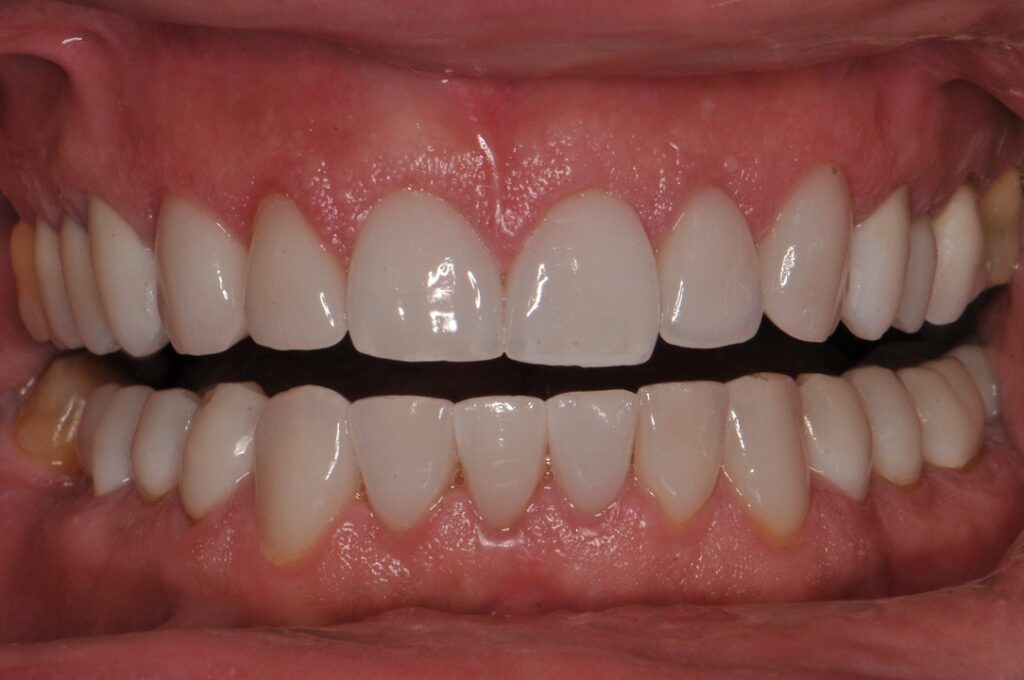
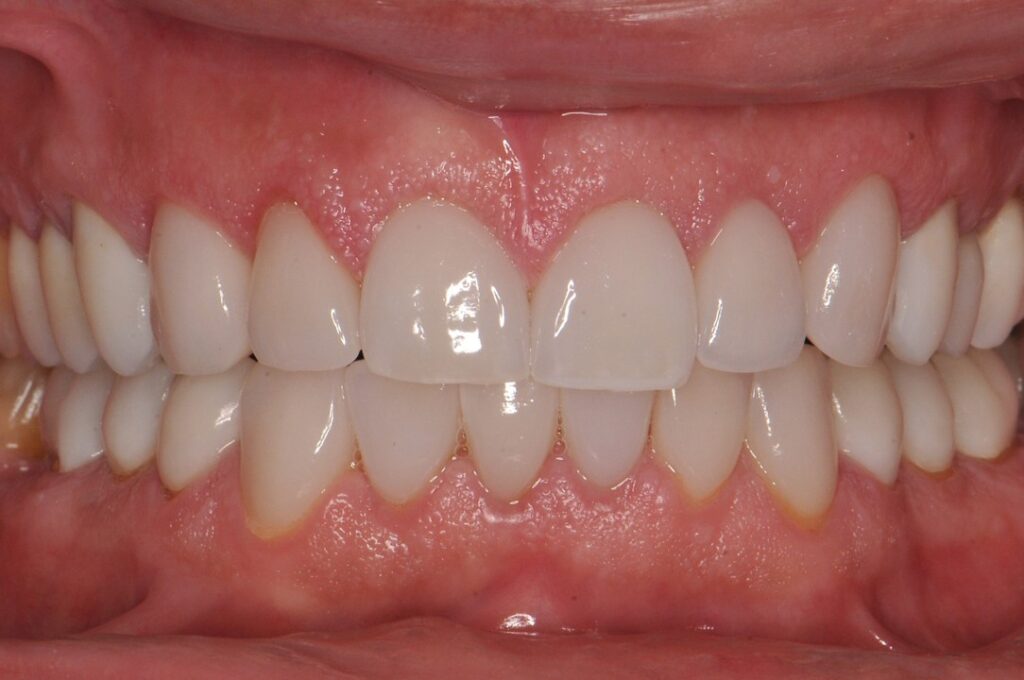
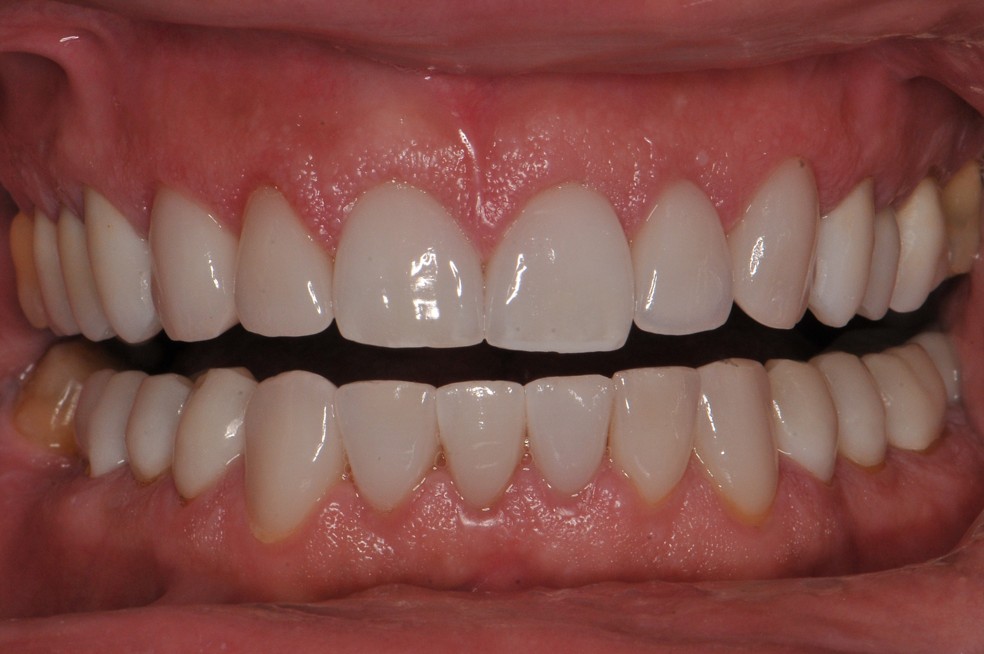

Why is proper occlusion important?
When the teeth come into contact in a balanced way, the mouth functions smoothly and without excessive stress. Proper occlusion helps:
with proper chewing and better distribution of forces
maintain the stability of teeth and restorations (fillings, crowns, bridges, implants)
protect teeth from wear, cracks, or fractures
reduce strain on the muscles and the temporomandibular joint (TMJ)
support the long-term health of the gums and periodontal tissues
What may indicate an occlusion problem?
Some common signs we evaluate in the clinic are:
pain or a feeling of “fatigue” in the jaw, especially in the morning
headaches or pain in the temples
“clicking” or grinding in the jaw joint
teeth grinding/clenching (bruxism)
tooth sensitivity without an obvious cause
wear or flat surfaces on the teeth
breakage of fillings or restorations that frequently become loose
a feeling that the bite is “not closing properly” or that one tooth contacts first
How is occlusion evaluated?
The evaluation is clinical and personalized. It typically includes:
assessment of contact points using special articulating paper
evaluation of jaw movement and the temporomandibular joint (TMJ)
assessment of wear, cracks, and areas of excessive load
when needed, digital recording or analysis using study models/scans
evaluation of occlusion before and after treatments such as crowns, bridges, or implants
How is dysfunctional occlusion treated?
Treatment depends on the cause and severity. It may include:
a night guard (occlusal splint) to protect the teeth and relieve pressure on the muscles and joint
selective equilibration (minor adjustment of contact points), when indicated
orthodontic treatment in cases of malocclusion (e.g. crossbite, prognathism, crowding)
restoration of wear using composite resins or crowns when there is significant loss of tooth structure
careful planning of implant restorations to prevent overloading
Our goal is an occlusion that is functional, comfortable and stable, without putting a strain on teeth and joints.
When should you have your occlusion checked?
An evaluation is particularly useful when:
you have symptoms (pain, clicking, headaches, wear)
you are about to undergo extensive dental treatment (crowns, bridges, implants)
there is a history of bruxism
you notice changes over time in the way your bite “comes together”
Appointment
Comfort
Friendly environment
Quality of services
If you suspect that your occlusion is not balanced or you are experiencing discomfort in your jaw or teeth, a targeted evaluation can provide a clear diagnosis and personalized solutions tailored to your needs.